
2026 Medicare MFP Changes: What Pharmacies Need to Do and How PrimeRx Will Support You
On January 1, 2026, Medicare’s Maximum Fair Price (MFP) program introduced new pricing and reimbursement rules for select high-cost Medicare Part D medications. While your day-to-day dispensing workflow will remain familiar, how reimbursements are handled will change.
PrimeRx is preparing built-in tools and reporting to help pharmacies stay compliant, protect cash flow, and maintain accurate profit tracking.
What Is Medicare MFP?

The Medicare Maximum Fair Price (MFP) program establishes negotiated price caps for certain high-cost Part D medications. The goal is to reduce out-of-pocket costs for Medicare beneficiaries while ensuring pharmacies are reimbursed properly through manufacturer rebates.
What To Expect
- Manufacturers will reimburse pharmacies for the difference between the AWP and the MFP.
- This change shifts reimbursement workflows rather than altering dispensing processes.
- Pharmacies will need enhanced reconciliation and tracking of
manufacturer refunds. - PBMs and pharmacy software systems must support new billing, reporting, and audit requirements to remain compliant.
Why This Matters for Your Pharmacy
- Price negotiation: Medicare negotiates lower prices directly with manufacturers for select drugs with historically high utilization and spending.
- Patient impact: Patients pay less at the point of sale, improving medication affordability and adherence.
- Pharmacy workflow: Pharmacies continue normal purchasing and dispensing processes without disruption.
- Reimbursement change: Payment structure shifts so manufacturers provide post-dispense refunds to cover the MFP reduction.
- Financial protection: Assists pharmacies in mitigating financial loss, as they do not absorb the price decrease.
- Program outcome: MFP balances patient affordability, manufacturer accountability, and pharmacy sustainability within Medicare Part D
Drugs Currently Expected to Be Impacted
Subject to change based on CMS updates
Eliquis
Jardiance
Xarelto
Januvia
Farxiga
Entresto
Enbrel
Imbruvica
Stelara
NovoLog and Fiasp (insulin aspart products)
Required Action: Register for Medicare Transaction Facilitator (MTF)
CMS has created a rebate mechanism for MFP reimbursements. Pharmacies must register with the Medicare Transaction Facilitator (MTF) to receive post-dispense manufacturer rebates. If your pharmacy is not registered, you may not receive MFP reimbursements, which could result in financial losses on eligible prescriptions.
Beacon MFP
Unlike the Medicare Transaction Facilitator, Beacon MFP is not mandatory. However, NCPA advises that the system offers many capabilities that pharmacies may find helpful in navigating the new payment and reconciliation processes. A few of those capabilities, which exceed functionality offered through the MTF, include:
- Processing Status Details. Pharmacies can access real-time information about refund status. This includes visibility into each step in the refund process, which can be helpful should a problem arise. With increased visibility, a pharmacist can identify the exact point at which a processing delay occurred and focus on addressing the reason for the problem.
- Good Faith Inquiries. The platform includes a mechanism for pharmacies and manufacturers to resolve disputes through good faith negotiation. The Beacon MFP platform allows the two parties to exchange information and communicate about potential disputes, with a goal of resolving issues without having to file a formal complaint with CMS. The “good faith” provisions allow pharmacies to document their attempts to resolve issues, which is a prerequisite to escalating an issue to CMS.
- Basis of Pricing. The platform provides visibility into the processes used by manufacturers to determine refund values.
How the MFP Reimbursement Flow Works
Pharmacy purchases the drug at normal acquisition cost
Patient fills an MFP-eligible Medicare Part D prescription
Pharmacy submits the claim as usual
Plan reimburses based on the MFP amount
Patient pays a reduced cost
Manufacturer issues a rebate to the pharmacy
Pharmacy reconciles and tracks refunds for accuracy and audit readiness
How PrimeRx Supports MFP Workflows
An upcoming PrimeRx update will include built-in support for Medicare MFP processing.
Key Features Include
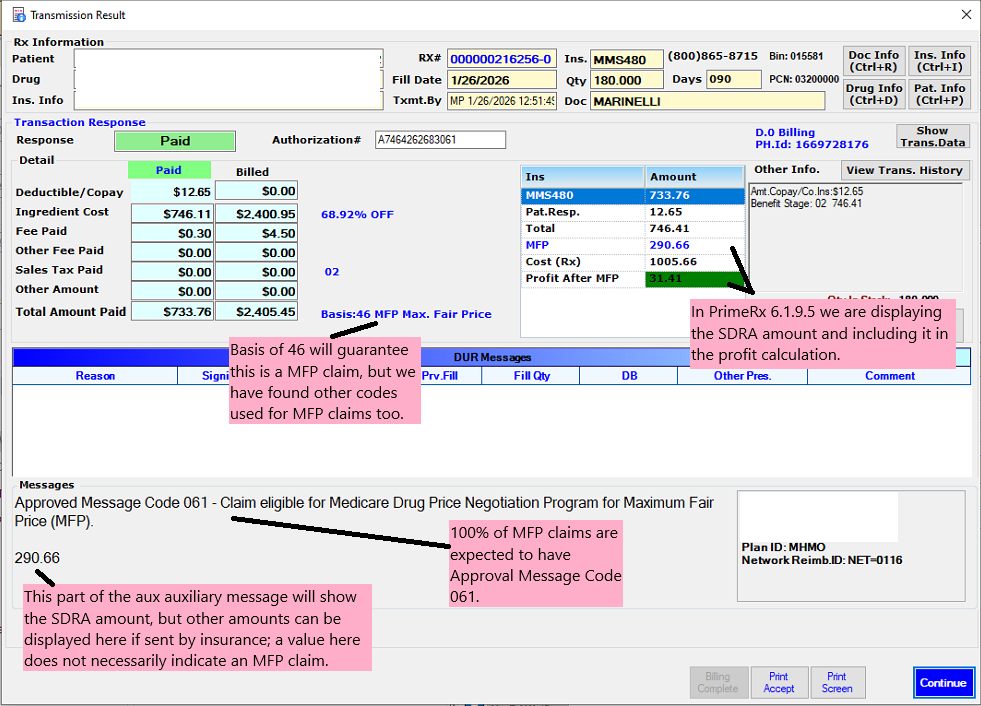
MFP details displayed directly in the pay record screen
MFP incorporated into profit calculations
Automated handling of MFP remittance tracking
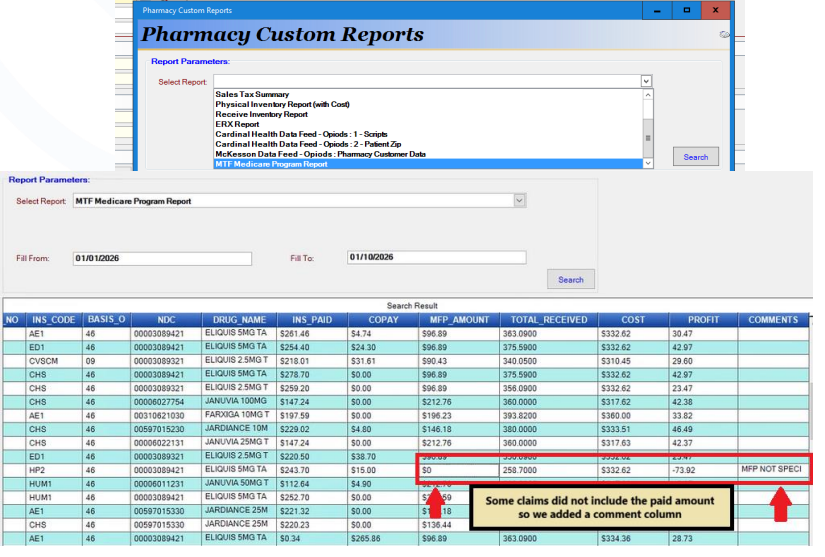
Enhanced reporting in Custom Reports to monitor MFP claims
Easy Identification of MFP Claims
Approved Message Code 061 will flag paid MFP claims
A new identifier tied to Basis of Reimbursement Determination (Field 46) will help recognize MFP transactions
PrimeRx will calculate true profit by including manufacturer rebate amounts
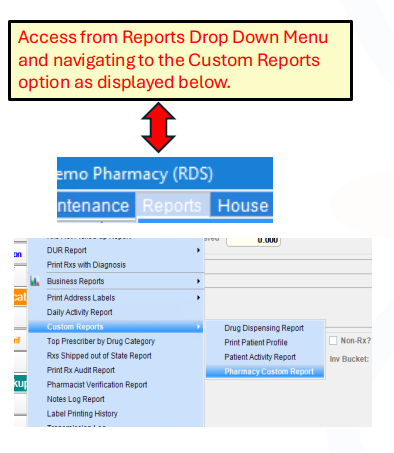
Custom Report
A new custom report deployed on 01/07/2026 will allow pharmacies to identify all MFP claims and see the correct profit. You can access it from the Reports drop-down menu by navigating to Custom Reports.
Training and Ongoing Support
- Training session booking link is here.
- Upcoming new release webinars will include information on the 2026 MFP program. Please note that our training webinars are hosted within the customer portal and require login access. Portal access is available to customers only.
- For upcoming webinars, please visit here.
- If you have any questions, please contact our Support team: [email protected]
